Treat Peyronie Disease: A Grounded, Practical Guide to Healing and Hope
Treat Peyronie Disease is not only a medical goal — it is often an emotional journey. When a man notices curvature, pain, or changes in erection quality, the impact goes beyond physical symptoms. It can affect confidence, intimacy, identity, and the nervous system’s sense of safety. Many men silently carry shame or fear, which amplifies stress responses and makes symptoms feel even more overwhelming.
The encouraging truth is that Peyronie’s disease is manageable. With accurate diagnosis, informed treatment choices, and supportive lifestyle changes, many men regain function and confidence. This guide explains how to treat Peyronie Disease using evidence-based approaches, practical tools, and psychological support — all in a grounded, realistic way.
Table of Contents – Treat Peyronie Disease
- Understanding Peyronie’s Disease
- The Psychological and Nervous System Impact
- Accurate Diagnosis and Medical Evaluation
- Non-Surgical Options to Treat Peyronie Disease
- Injectable and Prescription Therapies
- Traction and Vacuum Therapy
- Surgical Solutions
- Lifestyle and Holistic Support
- Communication and Intimacy Support
- Key Takeaways
- Frequently Asked Questions
Understanding Peyronie’s Disease
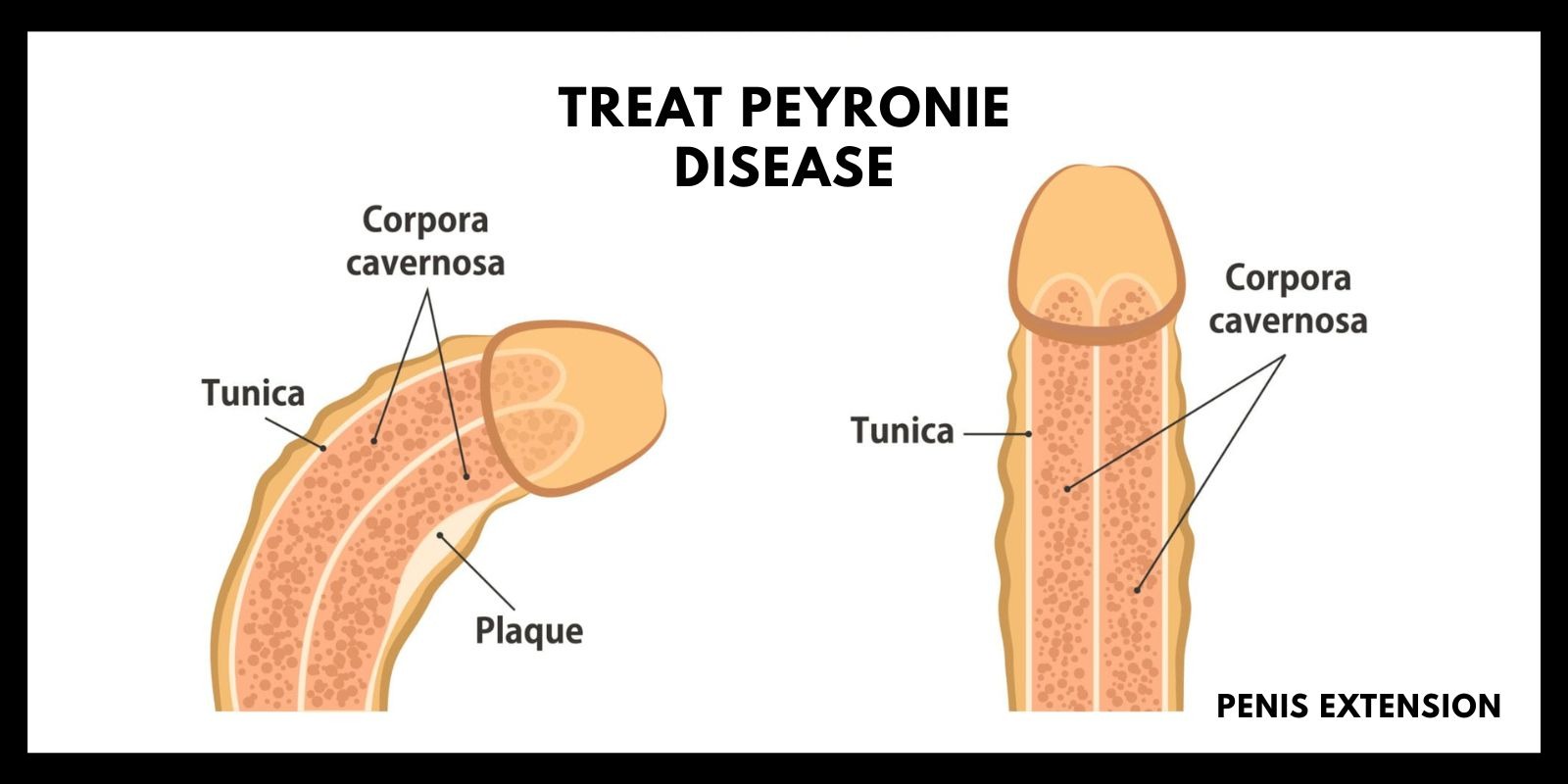
Peyronie’s disease develops when fibrous scar tissue forms in the tunica albuginea, the sheath surrounding erectile tissue. This scar tissue reduces elasticity, causing curvature, shortening, or indentation during erection. The condition may follow penile injury, repetitive micro-trauma, or genetic predisposition affecting connective tissue healing. While the exact cause is not always identifiable, inflammation and abnormal collagen deposition play central roles.
Symptoms often unfold in phases. The acute phase may include pain and evolving curvature, typically lasting over a year. The chronic phase follows, where pain subsides but curvature stabilizes. According to the Urology Care Foundation’s Peyronie’s Disease overview, treatment decisions depend on the phase and severity, which is why timing matters when planning to treat Peyronie Disease effectively.
The Psychological and Nervous System Impact
In my studies of men navigating sexual health challenges, one pattern I’ve noticed is how quickly the nervous system shifts into threat mode. Changes in erection or penile shape can trigger anxiety, which activates the sympathetic nervous system. Elevated stress hormones may worsen erectile performance, creating a cycle of worry and reduced function that compounds the physical issue.
Attachment patterns also influence how men cope. Those with avoidant tendencies may withdraw from intimacy, while others may become hyper-focused on performance. Addressing these emotional layers is not secondary — it is integral. When men feel safer and less ashamed, treatment adherence improves, and outcomes tend to be more positive.
Accurate Diagnosis and Medical Evaluation
To treat Peyronie Disease appropriately, accurate diagnosis is essential. A urologist typically performs palpation to identify plaque and may induce an erection using medication to measure curvature. Ultrasound imaging can assess calcification and blood flow, clarifying whether erectile dysfunction is also present.
Photographic documentation taken privately at home can help track progression. If erection quality is inconsistent, it is important to rule out other causes such as vascular issues or prolonged erections discussed in All You Need to Know About Priapism (Prolonged Erection). A thorough evaluation ensures treatment decisions are precise rather than reactive.
Non-Surgical Options to Treat Peyronie Disease
In mild or early cases, watchful waiting may be appropriate. Some men experience stabilization without aggressive intervention. During this period, doctors may recommend anti-inflammatory approaches or oral therapies, though evidence for many supplements remains mixed.
Vitamin E was historically prescribed due to its antioxidant properties. While low risk, its effect on curvature is modest. More recent clinical guidance, such as information outlined by the Mayo Clinic’s Peyronie’s Disease treatment guidelines, emphasizes individualized care rather than one-size-fits-all supplementation.
Injectable and Prescription Therapies
Collagenase Clostridium histolyticum is an FDA-approved injectable treatment designed to break down collagen within the plaque. This therapy is most effective for stable curvature exceeding moderate degrees. In carefully selected patients, measurable curvature reduction can occur over several treatment cycles.
Other medications such as pentoxifylline and interferon aim to reduce inflammation and scar progression. If erectile dysfunction coexists, reviewing options outlined in Comprehensive List of Prescription Pills for Treating Erectile Dysfunction may support overall function while plaque-focused therapies address curvature.
Traction and Vacuum Therapy
Penile traction therapy applies gentle, consistent stretching to encourage tissue remodeling. Over time, mechanical tension can promote length preservation and modest curvature improvement. One pattern I’ve noticed clinically is that consistency matters more than intensity. Gradual, structured traction tends to outperform aggressive use.
Devices such as medically designed extenders can support this process. Exploring structured systems like those described in Discover the Benefits of Male Edge Penis Extender may offer a non-invasive adjunct approach when supervised properly. Vacuum erection devices may also improve blood flow and support tissue oxygenation.
Surgical Solutions
Surgery is typically reserved for stable disease causing significant functional limitation. Options include plication procedures, plaque incision with grafting, or penile prosthesis implantation when erectile dysfunction is severe. Each carries benefits and trade-offs, including possible shortening or altered sensation.
Careful counseling before surgery is critical. Emotional readiness, realistic expectations, and understanding recovery timelines influence satisfaction rates. When surgery is thoughtfully chosen, it can restore sexual function and reduce psychological distress.
Lifestyle and Holistic Support
Systemic health influences connective tissue repair. Smoking cessation, cardiovascular exercise, balanced nutrition, and moderated alcohol intake improve vascular health, which supports erectile function. Diabetes and hypertension management are especially important because microvascular damage can worsen symptoms.
Stress reduction techniques — slow breathing, mindfulness, or somatic therapy — help regulate the nervous system. When inflammation decreases and blood flow improves, the body is better positioned to respond to medical treatment. Lifestyle shifts are not a cure, but they enhance resilience and recovery capacity.
Communication and Intimacy Support
Curvature and performance changes can create relational tension if unspoken. Honest communication reduces misunderstanding and prevents partners from internalizing the issue as rejection. Framing treatment as a shared health journey fosters connection rather than isolation.
In my experience, couples who approach treatment collaboratively often report stronger intimacy afterward. Exploring pleasure beyond penetration during recovery maintains closeness and reduces pressure while you treat Peyronie Disease with patience and clarity.
Treat Peyronie Disease with Confidence and Clarity
Choosing to treat Peyronie Disease is an act of self-respect. With informed guidance, realistic expectations, and supportive tools, improvement is possible. Whether you begin with traction therapy, medical treatment, or surgical consultation, consistent care builds momentum toward restored function and confidence.
Key Takeaways
- Treat Peyronie Disease early to prevent progression and preserve function.
- Accurate diagnosis determines whether non-surgical or surgical treatment is appropriate.
- Traction therapy and FDA-approved injections can reduce curvature in selected cases.
- Nervous system regulation and emotional support improve treatment outcomes.
- Lifestyle changes enhance vascular health and connective tissue recovery.

Frequently Asked Questions – Treat Peyronie Disease
Can Peyronie’s disease go away on its own?
Mild cases sometimes stabilize without intervention, but persistent curvature often requires treatment.
Is Peyronie’s disease caused by sexually transmitted infections?
No. It is not contagious and is unrelated to sexually transmitted diseases.
When is surgery recommended?
Surgery is considered when curvature is stable and significantly interferes with sexual activity.
Does traction therapy really work?
Consistent, medically supervised traction may improve length and reduce curvature in some men.
Can stress make symptoms worse?
Yes. Chronic stress can impair erectile function and amplify perceived severity, making holistic care important.